
Dr Justin Bui, Consultant Dermatologist.
Mohs micrographic surgery has been recognised as a highly effective option for the removal of certain skin cancers, because the very precise surgical technique can achieve up to a 99% success rate in preventing a recurrence of the tumour.
Consultant Dermatologist and Mohs specialist Dr Justin Bui, an AMA (WA) member, says the procedure also preserves the maximum amount of healthy tissue around the cancer and aims to minimise scarring.
Dr Bui says the other advantage is that the patient will leave the surgery with confidence that the histologic examination of their skin cancer has been completed on the day, rather than requiring further follow-up for pathology results. That’s because the dermatologist removing the tumour is also able to interpret the tissue samples in the laboratory to ensure no cancer cells remain.
Studies have shown that the recurrence rate for primary BCCs after Mohs surgery is 1.4% to 4.4%, compared to the 4.1% to 12.2% rate for standard wide excision.1,2,3
“In the scenario of a recurrent BCC,” Dr Bui says, “Mohs surgery is an effective option yielding recurrence rates of 2.4% to 6.7% in comparison to up to 13.5% if repeat wide excision is opted for.”
Dr Bui, who is the Honorary Secretary of the WA faculty of the Australasian College of Dermatologists, says an important first step in Mohs treatment is a biopsy of the skin cancer.
“This is so we can confirm that the target tumour is best treated with Mohs surgery,” he explains, “because the biopsy may reveal a diagnosis inappropriate for Mohs surgery – for example, lymphoma that’s presenting on the skin or an amelanotic melanoma – so you need to know that before proceeding.”




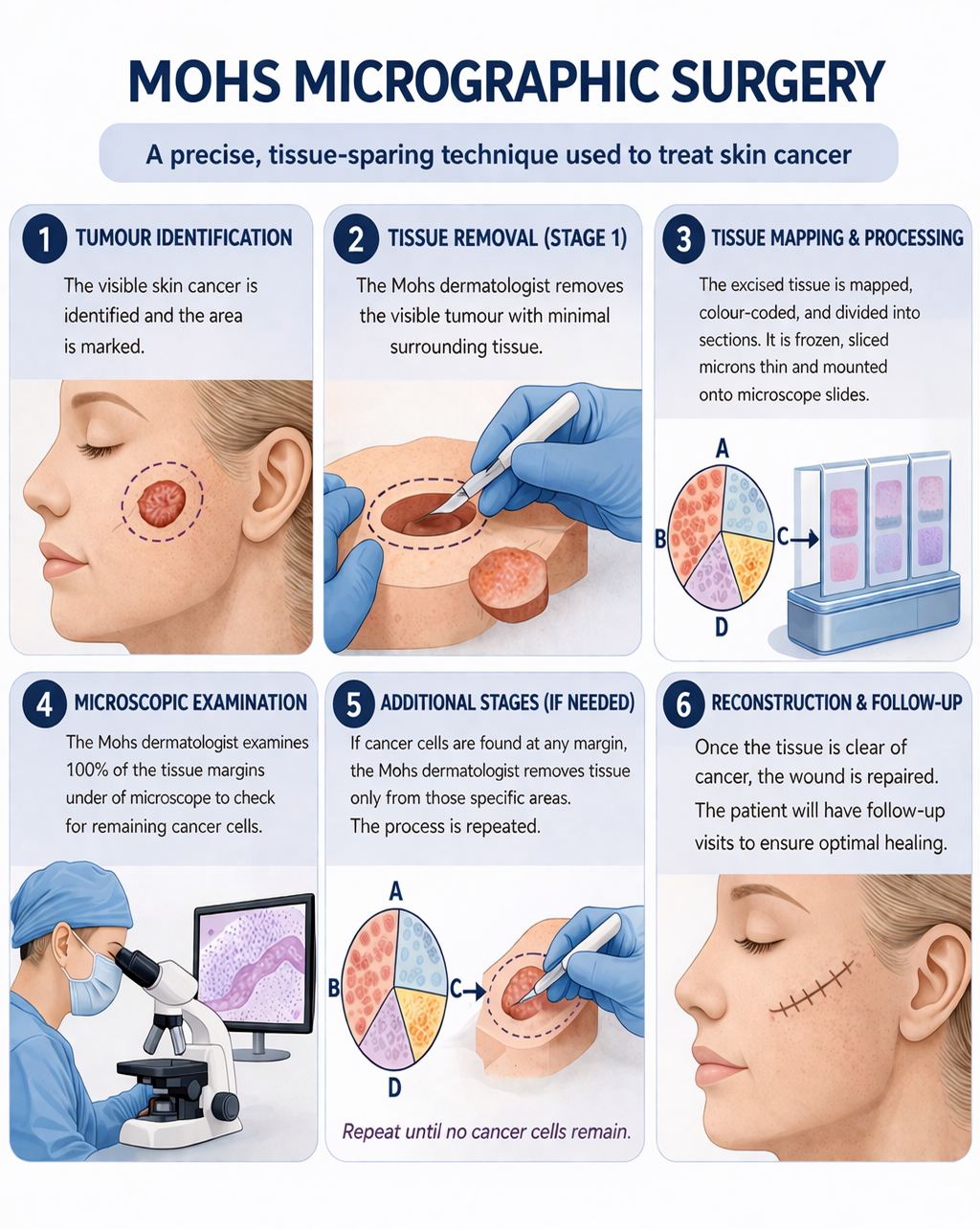 “The patient has local anaesthetic infiltrated and the tumour is then de-bulked using a curette or a scalpel, and that will provide us lesional tissue to correlate with the margins,” Dr Bui explains.
“The patient has local anaesthetic infiltrated and the tumour is then de-bulked using a curette or a scalpel, and that will provide us lesional tissue to correlate with the margins,” Dr Bui explains.