A multidisciplinary medical team at Sir Charles Gairdner Hospital (SCGH) has pulled off an Australian-first surgery on a patient with suspected lung cancer. Using a robotic bronchoscopy system, they were able to take a biopsy that confirmed the cancer and then remove it – all in a single operation, under one anaesthetic.

Dr Miguel Mesa-Guzman and Dr Dhaval Thakkar.
SCGH respiratory, pathology and surgical teams all combined to detect, diagnose and remove the woman’s cancer in an operation that lasted more than four hours.
Respiratory specialist Dr Dhaval Thakkar led the ground-breaking surgery that detected the cancer deep in the lungs, before carrying out precision tissue sampling, and then highlighted the cancerous nodule with a green, glowing marker which enabled thoracic surgeon Dr Miguel Mesa-Guzman to easily locate and remove it using keyhole surgery.
The “one and done” operation was made possible by the Ion robotic bronchoscopy system.
Developed by California-based Intuitive, the makers of Da Vinci robotic surgical systems, the Ion platform allows the biopsy of small, hard-to-reach nodules in the peripheral lung, where more than 70% are located.
Dr Thakkar, an AMA (WA) member, said CT and PET scans showed the patient, who had a history of lung cancer more than a decade ago, had developed a lesion in her other lung.
“We identified her as being a high-risk candidate for cancer because of the PET scan, her history, and what it looked like on radiology,” he said.
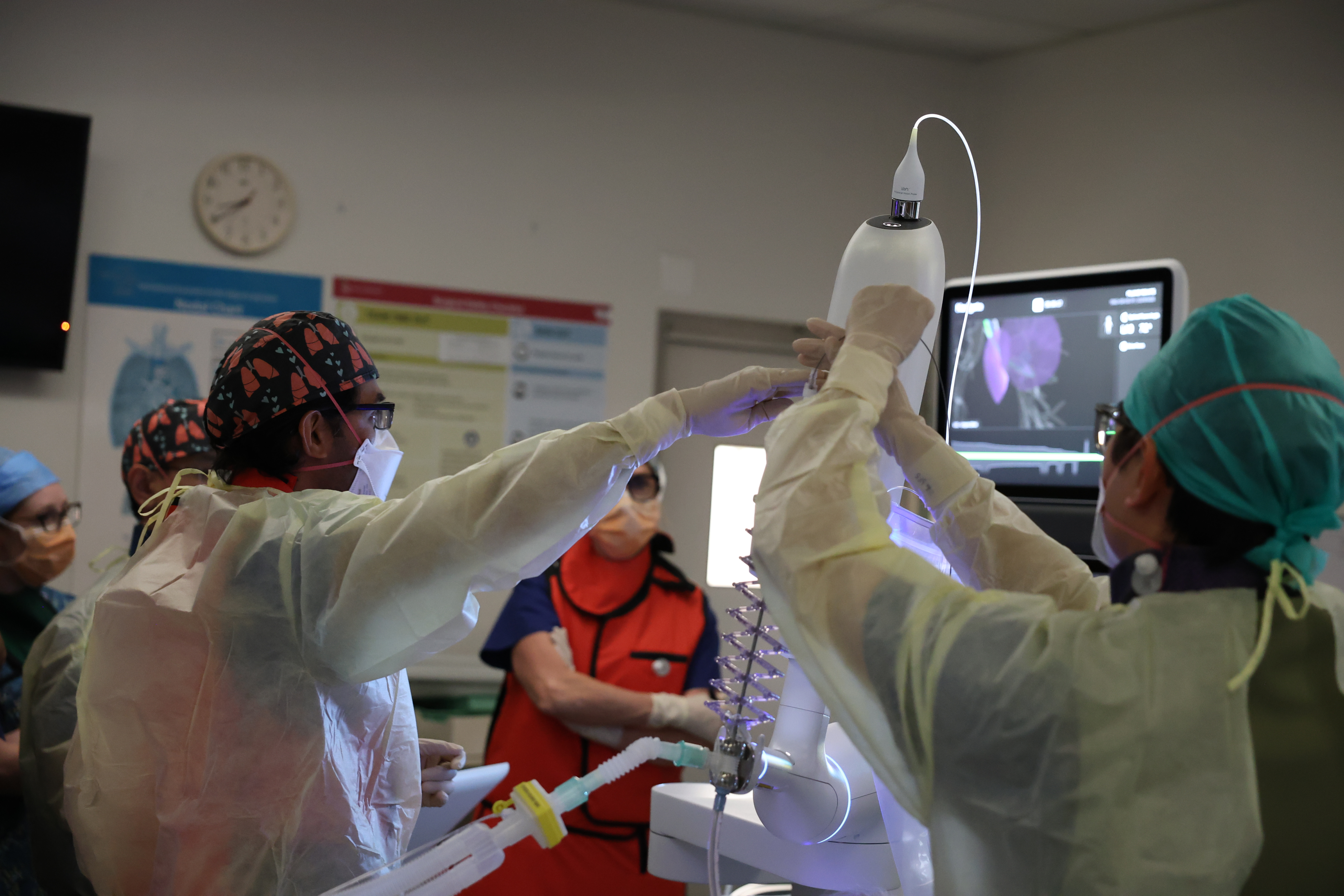
Detecting the cancer with the robotic bronchoscopy system.
“We reviewed it with Miguel. He saw the patient in the clinic, and we then offered her this option. Typically, what we’d do is biopsy and confirm before we go to surgery. But in this patient’s case, we decided we could do the robotic surgery.
“While she’s still under anaesthetic, I can go in and put a marker in for Miguel. I put in a coil that’s soaked with a chemical that glows green under a certain light. If I mark that exact location, then Miguel just cuts out everything that’s glowing. And with this case, because the patient already had a lung resection, we wanted to take out only what was absolutely necessary.
“In the last few years, we’ve had data saying we can cut less than the internal lobe. We have five lobes in the lung: three on the right, two on the left. And we’ve historically just done lobectomies. But recently we’ve had studies that suggest you can cut out less than a lobe, and the outcomes are just as good.”
For the operation, the CD scan was fed into the Ion system to create a 3D representation of the patient’s lungs.
“Then, on a laptop that we have, we tell the robot where we want to target, and frequently it will figure out what the margins of it are,” Dr Thakkar explained.
“Sometimes we have to draw them in, depending on what the lesion looks like, and it can identify the margin. But we tell the robot where we want to target, and it will go through the airway map and generate the best pathway. Sometimes that’s not the best pathway, and we have to then instruct it for a better pathway. So there’s still a human component to it, but the robot’s pretty darn good.”
Dr Thakkar says the robotic system, using a 3.5mm wide catheter into the lung, improves diagnostic yield with fewer complications. This can save a patient from needing follow-up procedures, thereby reducing the time in hospital and getting treatment quicker.





